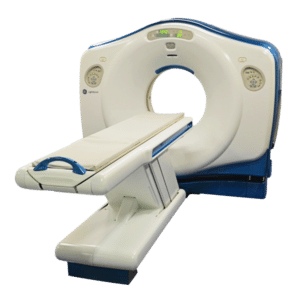
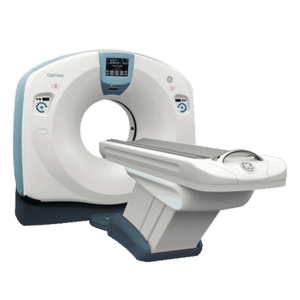
Amber Diagnostics has an extensive selection of high-quality refurbished and used CT scanners for sale at competitive prices
Mobile Options
Mobile CT Scanners
Our top-tier CT scanners are available to ensure seamless patient care and uninterrupted diagnostics.
For RentalFor Sale
Featured
Our Most Requested
CT Scanners
Choose The Best
Why Amber Diagnostics Used CT Scanners?
Since 1994 Amber Diagnostics has offered a wide array of quality refurbished and used CT Scanners for sale. In our 25,000 square foot warehouse we offer end to end service for every preowned equipment we house. We have installed CT scan machines for urgent care facilities, outpatient departments, private practices, and major medical centers throughout the world.
During your consultation, our equipment experts will discuss your department’s needs, budget, and space requirements. We will support you in every stage of the process; from site planning to shipping, installation and technical servicing. Keep your costs down and imaging capabilities high with Amber Diagnostics.
Contact Us Today