MRI technique to help identify MS (multiple sclerosis) patients that are at most risk for developing a physical disability
A recent study conducted by the University of Buffalo discovered that they were able to use an advanced MRI technique to help identify MS (multiple sclerosis) patients that are at most risk for developing a physical disability due to their condition.
The technique is called “quantitative susceptibility mapping,” and lead author Robert Zivadinov hopes it can provide a better way of identifying patients at risk of cognitive and physical decline, as the method currently being used leaves something to be desired when it comes to accuracy.
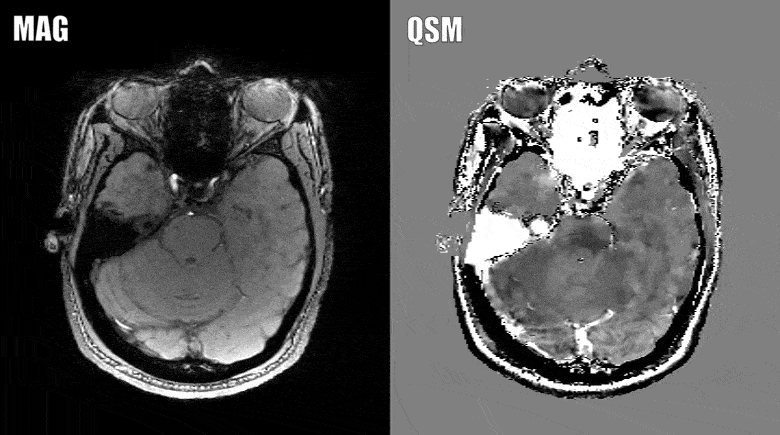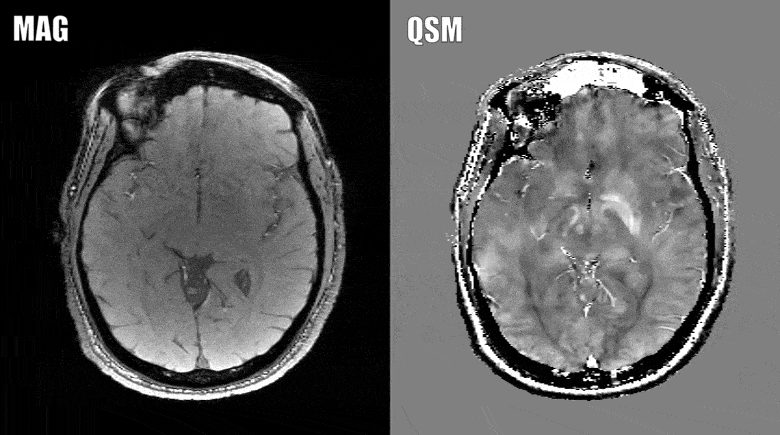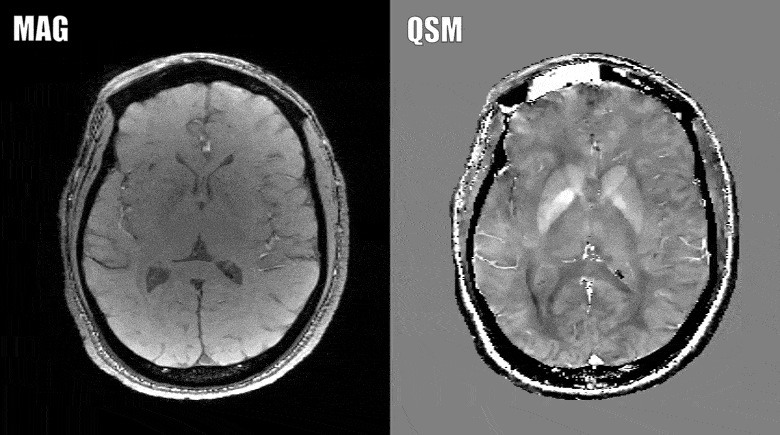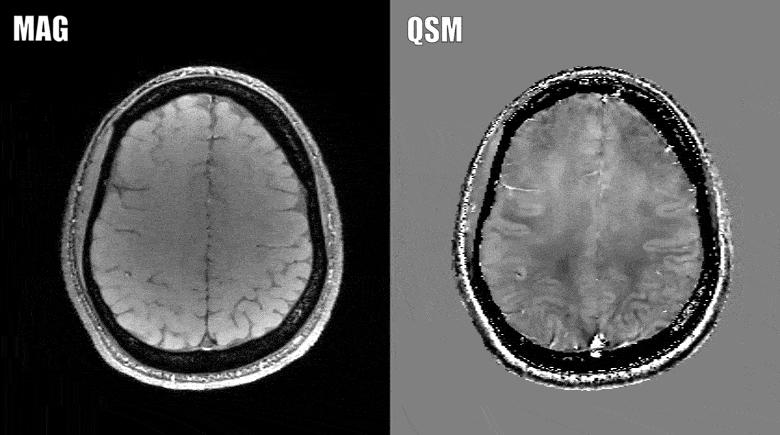
The presence of brain atrophy is currently the gold standard when it comes to predicting this decline. The problem is that brain atrophy is difficult to see, and an earlier measure of exactly who will eventually develop MS related disability is needed, which is where the advanced MRI method comes in.
Three key central nervous system components are attacked in patients with MS. Nerve fibers, myelin, and Schwann cells (which produce myelin). Common symtpons are pain, spasticity, and weakness in the patient, and many of those with disease progression develop severe disability.
Quantitative susceptibility mapping assesses the iron levels in the brain, which may provide better clues and measures of what exactly happens to a brain with MS as the disease progresses.
Increased and decreased iron amounts in the brain can be damaging, but iron is required for a variety of functions within brain cells (including myelination).
Says lead author Robert Zivadinov, “It is known that there is more iron in the deep gray matter structures in MS patients, but also we’ve seen in recent literature that there are regions where we find less iron in the brains of these patients.”
Get Started
Request Pricing Today!
We’re here to help! Simply fill out the form to tell us a bit about your project. We’ll contact you to set up a conversation so we can discuss how we can best meet your needs. Thank you for considering us!
Great support & services
Save time and energy
Peace of mind
Risk reduction
Zivadinov and his colleagues used the MRI technique to study the iron levels in the brains of 600 MS patients (452 with early-stage disease and 148 with disease progression) as well as 250 healthy controls.
The technique showed that a higher iron concentration in the brain meant a higher magnetic susceptibility, while a lower concentration of iron in the brain meant lower susceptibility.
MS patients, in comparison with the control group, showed higher levels of iron in the basal ganglia (essential for movement), and lower levels in the thalamus (essential for sensory input processing).
These patients with MS that showed high levels of iron in the basal ganglia and lower levels in the thalamus were associated with longer duration of the disease, disease progression, and greater degrees of disability.
According to the author, this is the first time a study has shown increased iron levels in the basal ganglia, but decreasing in the thalamic structures of MS patients.
“Iron depletion or increase in several structures of the brain is an independent predictor of disability related to MS,” Zivadinov added. He also noted that the studies findings could provide a future role for quantitative susceptibility mapping when it comes to clinical trials of new drugs. “Susceptibility is an interesting imaging marker of disease severity that can predict which patients are at severe risk of progressing. To be able to act against changes in susceptibility would be extremely beneficial.”